At present, elastomeric impression materials and dental stone are still used to prepare master models for RPDs with casting framework. The clinical adaptation of prosthesis may be affected by factors, such as the physical and chemical properties of materials, practitioner’s proficiency, indoor environmental conditions, the possible wear of the models in logistics, etc, however, the influences of the above factors on the accuracy of restoration can be avoided by the digital impression method [6]. Many studies had confirmed that the clinical adaptation of fixed prosthesis fabricated on 3D printed resin models by using digital impressions was better than that on the dental stone models [7, 8]. However, the replication accuracy of digital impression for a large range of edentulous alveolar ridge needed to be improved in clinical practice[9]. The working area of impression for removable denture was much larger than that for fixed denture. This study aimed to guarantee the accuracy of digital impression for defected dentition according to the working principle of digital intraoral scanner and the characteristics of taking impression for removable denture, and the following factors that may affect image acquisition effect in the process of taking digital impression needed to be controlled. Firstly, saliva and other body liquids covering soft and hard tissues in oral cavity needed to be aspirated at any time, and especially saliva in mouth floor needed to be controlled when scanning lingual surface of mandible. Due to light reflecting on the liquid surface and formation of blank image, the image of oral tissues was not captured by the scanning head, and the system failed to recognized the morphology of the object, which led to the scanning procedure suspended or data lost. Therefore, the traditional method of taking elastomeric impression was still applied to the cases that saliva in mouth floor could not be controlled. Secondly, the surface of mucosa should be kept moist.
The image of oral soft tissue was not captured by the scanning head, and the scanning procedure was suspended if the mucosal surface was overdried. Thirdly, the scanning head should be parallel to the surfaces of the scanned objects and be kept a certain distance when the smooth and shiny surfaces, such as the surfaces of ceramic and metal prosthesis and worn teeth, were scanned. Clinging to the surfaces of the objects should be avoided. Fourthly, the mouth mirror and the saliva ejector were used to appropriately pull and push soft tissues, including lips, tongue, buccal tissue, and mouth floor, to imitate muscle functional trimming when the mucogingival junction area was scanned. The oral frenum and the mucosal area outside the mucogingival junction should be included in the scanning range. The image of the frenum configuration, the light pink attached gingiva and red mucosa was clearly displayed on the screen, the prosthodontist or the dental technician was convenient to modify the impression image. Lastly, data of partial dentition needed to be acquired in most fixed restoration, and the scanning difficulty was low. However, data of soft and hard tissues of the whole dentition relevant to RPDs should be acquired in this study. Therefore, a reasonable order should be followed when scanning, in order to efficiently acquire image data of oral tissues and avoid missing data.
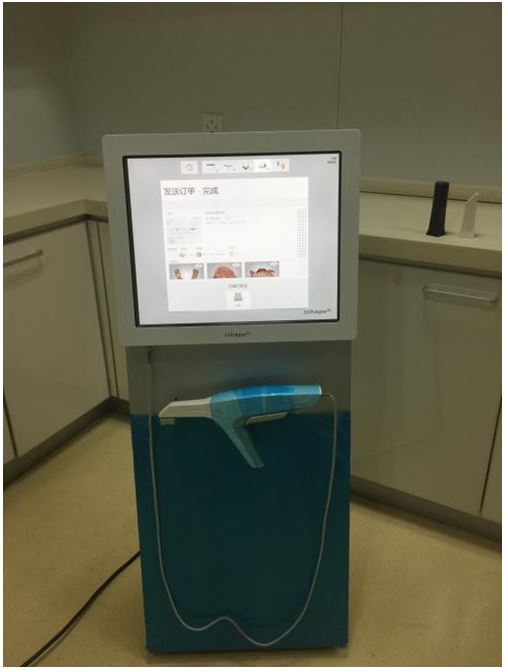
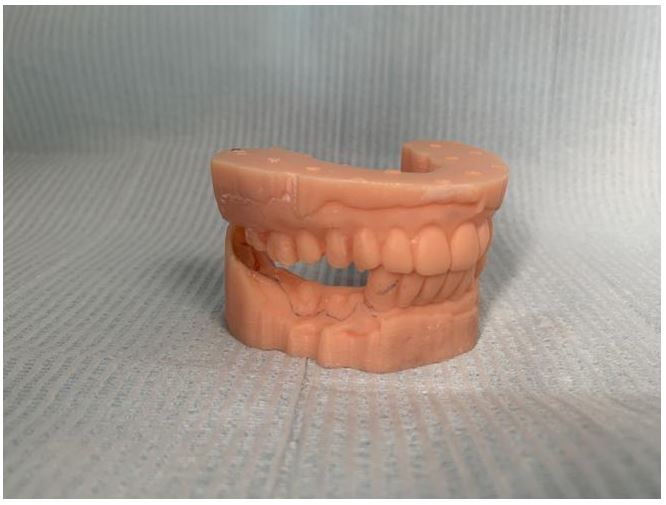
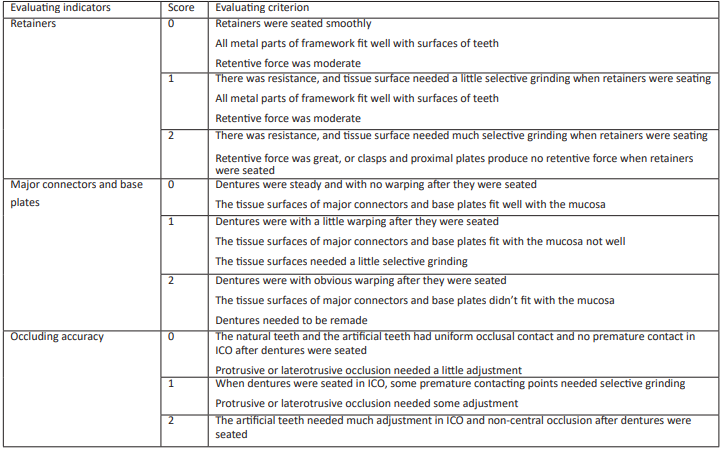
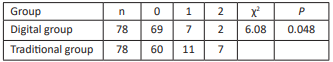
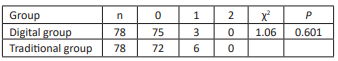
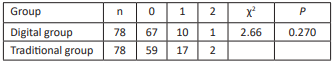
Data of digital impression collected directly from the patient’s mouth were stored in the scanner computer and sent to the dental lab via internet. Intraoral data were received and modified if necessary by the technician, and then the master resin models were fabricated in 3D printer. RPDs with bilateral retainers in this study were fabricated with the method of intraoral digital scanning combined with 3D printing resin models, and the clinical evaluation showed that the adaptation of retainers, including clasps, proximal plates and occlusal rests, and the occluding accuracy of RPDs with the digital method were better than those of RPDs fabricated with the traditional method. The possible reasons analysed were as followed: firstly, although the deformation rate of silicon rubber impression material was much less than that of alginate materials, silicon rubber impression still had permanent deformation amount of 0.2% -0.3%. Furthermore, silicon rubber impression could be affected by surrounding factors, such as temperature, disinfectant, etc. Therefore, the accuracy of prosthesis fabricated on the models made of the traditional materials was easy to be affected. However, the way to transfer digital data was not easy to be affected by the above factors[10]. Secondly, the tray bearing impression material was placed into patient’s mouth, which could lead to saliva increasing, violent activities of tongue and soft palate, etc. The accuracy of the impression was affected by these factors. Thirdly, Pure expansion phenomenon could happened in the process of dental stone hardening, and the expansion rate was about 0.085%. In addition, the range of crystal particle size of dental stone model was 12-25μm, and the crystal was prismatic or irregular in shape. However, compared to dental stone crystal, the particle of 3D printing resin material was smaller and well-distributed, and the capability of duplicating delicate structure was better. Fourthly, defects in various parts could be produced in the process of making dental stone models, and the risk of wear existed when storing and transferring models. Fifthly, master models were possible to be damaged in the process of fabricating RPDs. Lastly, the stable occlusal record in ICO could be acquired by intraoral digital scanning at the first visit, but the maxillomandibular relationship was recorded at the second visit in the most cases with dentition defect when the traditional method was used. In this study, there was no significant difference in the clinical adaptation of major connectors and base plates of RPDs fabricated with two methods. The reason analyzed could be that the risk of wear or damage to the edentulous alveolar ridge and the palate on the master model was smaller compared to the prominent part of the dentition.
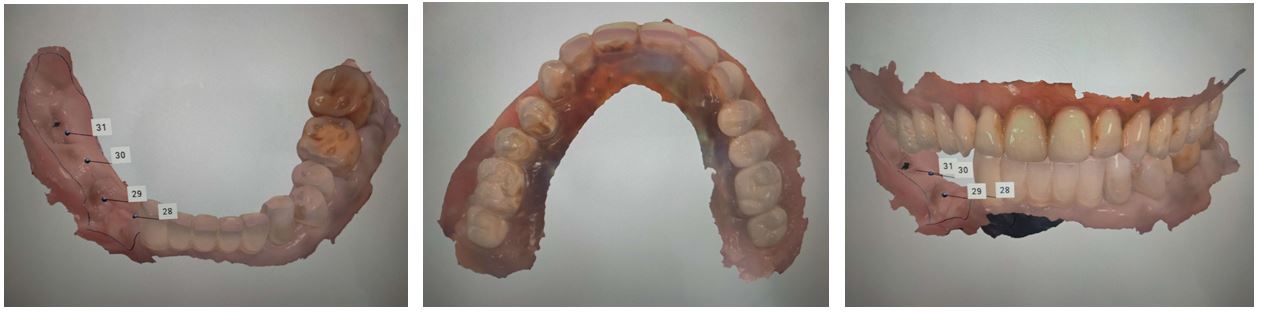
It was one of the technical difficulties in this study how to take digital selective pressure impression for the dentition with posterior free end edentulous area. The tissue structure of the dentition with posterior free end edentulous area was more complicated than that of with non-free end edentulous area. Under the normal occlusal force, the physiological mobility of healthy natural tooth was about 30μm, and the amount of vertical deformation of the alveolar mucosa in posterior edentulous area was up to 0.14-0.35mm. If RPDs were fabricated by using anatomical impressions, the adverse torsion could happen to the abutment teeth adjacent to free end edentulous area and damage periodontal health of the natural teeth when the free end of RPDs was under occluding force. Meanwhile, when the free end saddle subsided, the stress on the alveolar ridge was not well-distributed, which easily caused rapid absorption of alveolar bone and damaged mucosal tissue in edentulous area. Accordingly, the iatrogenic damage of oral hard and soft tissues and the restorative treatment failure in a short period arose. This study referred to the conventional method of taking selective pressure impression [6], and the method of combining wax block with bite registration material, which was easy for clinically operating, was used. Before intraoral digital scanning, mucosa was pressed for 30 seconds, which imitated functional occlusion in free end edentulous area. Then scanning mucosa in edentulous area should be completed rapidly (within 10 seconds) before mucosal deformation was restored. The experiment results showed that the method of taking digital selective pressure impression was clinically feasible to fabricate RPDs for dentition defect of Kennedy Class I and Kennedy Class II. Because the border of the base plate in edentulous area was hard to determine accurately on the scanner screen, and the method of taking digital selective pressure impression in this study was difficult to implement, the cases with mandible dentition defect of Kennedy class I were not included and discussed in this study.
As mentioned above, when dentition defect was restored with RPDs, compared to the traditional method, intraoral digital scanning and 3D printing resin model could improve the quality of prosthesis. Also, the stable central occlusal relation could be acquired by intraoral digital scanning at patient’s first visit, which reduced patient’s visiting times, operating steps and the chance of error in prosthodontic treatment[11-13].
Acknowledgements: Not applicable.
Funding: The authors received no financial support for the research, authorship, and/or publication of this article.
Competing interests: The authors state that there are no conflicts of interest to disclose.
Data availability: The authors declare that all data supporting the findings of this study are available within the paper and any raw data can be obtained from the corresponding author upon request.
Contribution of authors: (I) Conception and design: Lili Fan, Nan Zhang; (II) Administrative support: Nan Zhang; (III) Provision of study materials or patients:Yanyan Liu; (IV) Collection and assembly of data:Ruifeng Cao ; (V) Data analysis and interpretation: Guohu Zhao, Nan Zhang; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors.