An unusual case of left atrial “Mass”
Andreas Tassopoulos1, Maria Mouratidou2, Constantinos H Papadopoulos2
1Cardiology Department, Iaso General Clinic, Athens, Greece
2Laboratory of Echocardiography, 2nd Department of Cardiology, Korgialenio –Benakio, Red Cross General Hospital, Athens, Greece
*Corresponding author
*Ashwin Singh Chouhan , Cardiology Department, Iaso General Clinic, Athens, Greece
DOI: 10.55920/JCRMHS.2023.04.001142
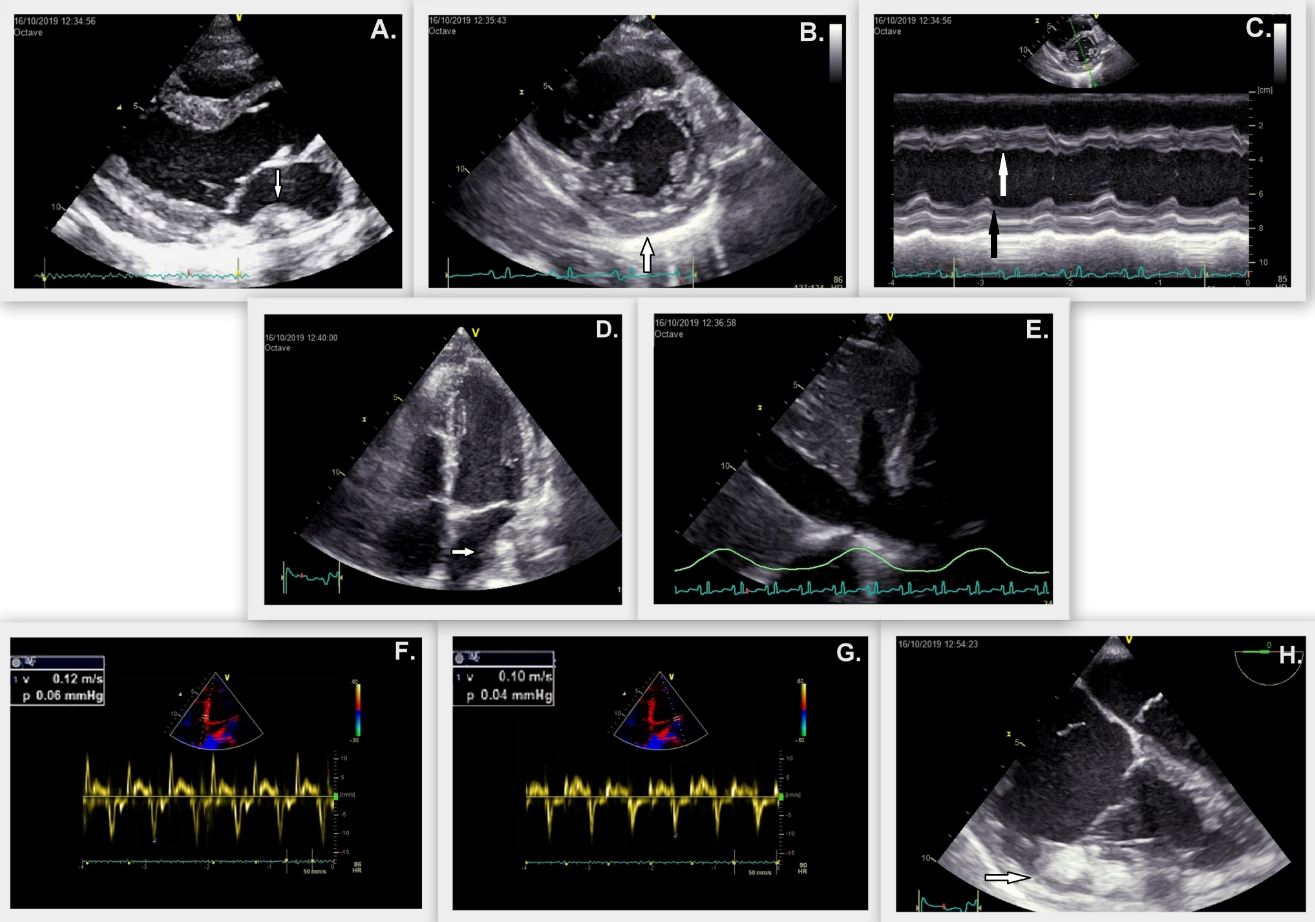
Figure 1- Initial echocardiographic study: A. Parasternal long axis view. Echodense mass at the posterolateral wall of the left atrium that projects into the left atrial chamber (arrow). B. Parasternal short axis view. Thickened pericardium with echodense content (arrow). C. M-mode echocardiography of the left ventricle. Bouncing motion of the interventricular septum (white arrow) and diastolic flattening of the posterior wall (black arrow). D. Apical 4-chamber view. Left atrial mass of equal echodensity as the pericardial content. E. Subxiphoid view. Dilated inferior vena cava. F and G. Tissue doppler measurement of medial (F) and lateral (G) myocardial tissue velocity. Mitral lateral e′ velocity is lower than the medial e′ velocity (“annulus reversus”). H. Transoesophageal four-chamber view. Echodense pericardial content (arrow).
Figure 2: Thoracic CT scan. Encysted pericardial effusions (arrow).
Figure 3: Echocardiographic study 3 months after the first study: A. Parasternal long axis view. Decreased volume of the aforementioned left atrial mass (arrow). B. Parasternal short axis view. Significant reduction in the pericardial thickness and the volume of the pericardial content (arrow). C. M-mode echocardiography of the left ventricle. Absence of the previously observed septal bounce and of the diastolic flattening of the posterior wall D. Apical 4-chamber view. Elimination of the previously detected left atrial mass. E. Subxiphoid view. Inferior vena cava of normal diameter. F and G. Tissue doppler measurement of medial (F) and lateral (G) myocardial tissue velocity. Equal mitral lateral and medial e′ velocities (absence of the “annulus reversus” pattern, gradual return to normal).
The patient was diagnosed with constrictive pericarditis, underwent pericardial biopsy (guided by pericardioscopy) and was put under treatment for a possible tuberculosis infection, due to his origin from an endemic area, his atypical symptoms and echocardiographic/ CT findings. The empiric antituberculosis treatment included four anti-TB drugs and adjunctive steroids, according to the current guidelines.1 However, the findings of the histopathological examination were consistent with non-specific inflammation, without signs of malignancy or granulomatous inflammation. The QuantiFERON test, as well as PCR and cultures in gastric fluid and pericardial content came out negative for Mycobacterium tuberculosis. Therefore, anti-TB treatment was halted except from steroid administration which was continued in conjunction with colchicine. After the improvement of his clinical condition and the normalization of the inflammatory markers, the patient was discharged 30 days after his admission, with instructions for regular follow-up.
The follow-up echocardiographic examination, one month after patient’s discharge, showed an improved left ventricular systolic performance, without the bouncing motion of the interventricular septum, the “annulus reversus” pattern and the dilated inferior vena cava that had been observed in the previous study. The thickness of the pericardium, the volume of the pericardial content and the size of the left atrial mass had been reduced compared to the previous study (Figure 3). These findings supported the diagnosis of transient constrictive pericarditis, considering the fact that empiric anti-inflammatory treatment reversed the pericardial constriction. Therefore, the patient was decided to continue the anti-inflammatory treatment with a careful tapering plan. The reduction of the aforementioned mass size also suggests that this finding likely represented inflammatory content in the oblique pericardial sinus that projected in the left atrium. This specific presentation of a solely echodense oblique sinus mass is an unusual finding. In most cases of oblique sinus (pseudo)masses, pericardial effusions within the oblique sinus permit the fat of the posterior atrioventricular groove to “pop out”, hence the simultaneous presence of a hyperechoic and an echo-free space is observed. These masses are usually detected with transthoracic imaging, whilst transoesophageal echocardiography is of limited value because the posterior wall of the left atrium is often not visualized in its entirety.2 This case indicates that the sinuses of the pericardium should be included in the differential diagnosis of cardiac masses, especially in the simultaneous presence of pericardiac diseases.
Conflicts of Interest and Source of Funding
None declared.
- Adler Y, Charron P, Imazio M, et al. 2015 ESC Guidelines for the diagnosis and management of pericardial diseases: The Task Force for the Diagnosis and Management of Pericardial Diseases of the European Society of Cardiology (ESC)Endorsed by: The European Association for Cardio-Thoracic Surgery (EACTS). Eur Heart J 2015; 36: 2921-64. doi: 10.1093/eurheartj/ehv318
- Penmasta S, Silbiger JJ. The transverse and oblique sinuses of the pericardium: Anatomic and echocardiographic insights Echocardiography 2019; 36: 170-6. doi: 10.1111/echo.14211