An 86-year-old man, with no known comorbidity, presented with a five-day history of colicky abdominal pain, worsening distension, and associated constipation which progressed to obstipation. The pain worsened significantly but with no associated vomiting. His last bowel movement was 4 days before presenting to the hospital. There was no history of fever, jaundice, early satiety, spurious diarrhea, the passage of pellet-like stools, or weight loss.
At admission, he was pale, not dehydrated, and tachycardic with a pulse rate of 120 per minute. His blood pressure was consistently high from presentation although he was not previously diagnosed as hypertensive. His abdomen was markedly distended with a midline longitudinal scar and hypoactive bowel sounds. There was no rebound tenderness. A digital rectal examination revealed scanty hard feces.
Past medical history showed he had a similar presentation fourteen months prior, with complaints of recurrent, worsening abdominal distension over a preceding 6 months period with associated pain, anorexia, and weight loss. Abdominal radiograph and ultrasound scan confirmed abdominal distension with volvulus.
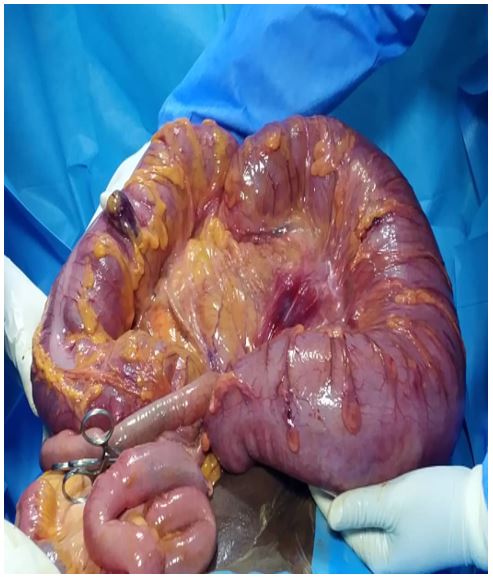
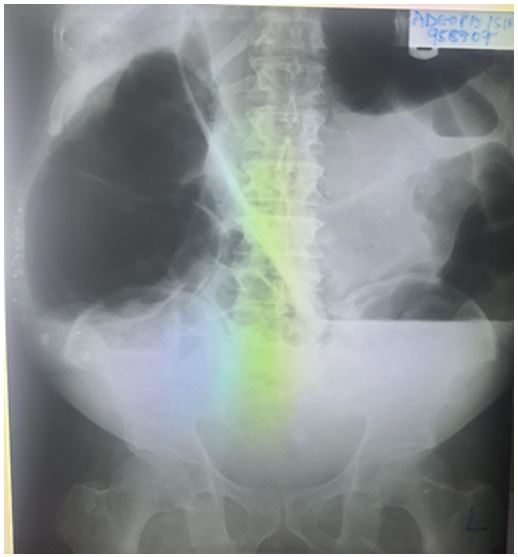
The full blood count revealed neutropenia and eosinophilia. Further workup tests for surgery were all within normal limits, including the electrolytes, urinalysis, and clotting profile. A plain abdominal x-ray revealed the classic omega sign (shown in Fig. 1). He had an exploratory laparotomy and the findings were markedly dilated sigmoid colon rotated about 2700 anticlockwise along its mesentery and it appeared pink and normal and contained hard feces (shown in Fig. 2). The caecum, ascending colon and transverse colon were noted to be mildly dilated. He had a one-stage sigmoidectomy with end-to-end anastomosis
With the current admission, a provisional diagnosis of adhesive bowel obstruction was made. Resuscitation was commenced with a nasogastric tube passed for immediate decompression. Evaluations were done to rule out a possibility of a second volvulus in this patient or Ogilvie syndrome as a second alternative. He was rehydrated with intravenous fluids and had a trial of enema done with minimal improvement.
He had a normal white cell count with a neutrophil predominance of 80.6% and a hematocrit value of 39.3%. Biochemical parameters were essentially normal except for a potassium level of 3.0mmol/L which was corrected before surgery. Viral markers were all negative and the clotting profile was not deranged. Urinalysis showed proteinuria, ketonuria, and haematuria. He had an erect abdominal radiograph done which showed multiple air-fluid levels and a gasless pelvis and a supine view showed massively dilated (>10cm) bowel loops peripherally located, with haustra markings (shown in Fig. 3).
Carcinoembryonic antigen was not elevated. Glycated hemoglobin was done after random plasma glucose was noted to be elevated. This was normal -5.9%. There were no abnormalities on the plain chest radiograph. His ejection fraction on echocardiography was 67%.
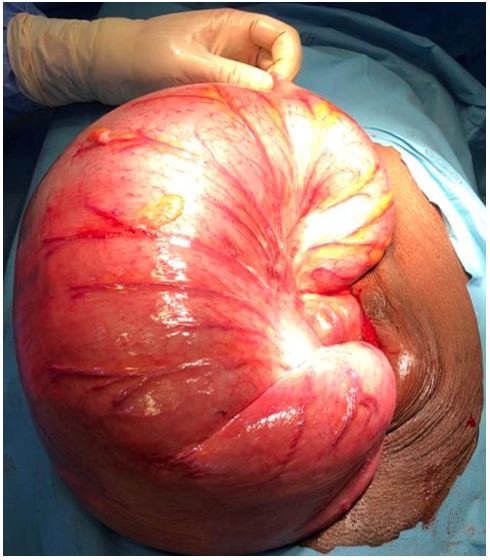
He underwent an exploratory laparotomy after the correction of hypokalaemia. Intraoperatively, findings included a massively dilated transverse colon that was twisted 5400 in the anticlockwise direction, perforation in the descending colon with spillage of intestinal contents (shown in Fig. 4). The bowel was viable and a left hemicolectomy was done with one-layered end-to-end anastomosis using 2-0 VicrylTM.
Following surgery, the clinical course was uneventful and he was discharged home 8 days after surgery.