Multivessel Coronary Artery Disease and Coronary Calcification in Patients with Ischemic Heart Disease:An Interventional Cardiologist’s Perspective
Nagaeva G.A*, Mukhammedova M.G, Yarbekov R.R, Muradov M.M, Khaidarova N.U, Tashmirov Zh.B
Research Center for Military Medicine of the Military Medical Institute of the University of Military Security and Defense of the Republic of Uzbekistan.
*Corresponding author
Nagaeva G.A, Research Center for Military Medicine of the Military Medical Institute of the University of Military Security and Defense of the Republic of Uzbekistan.
DOI: 10.55920/JCRMHS.2026.14.001588
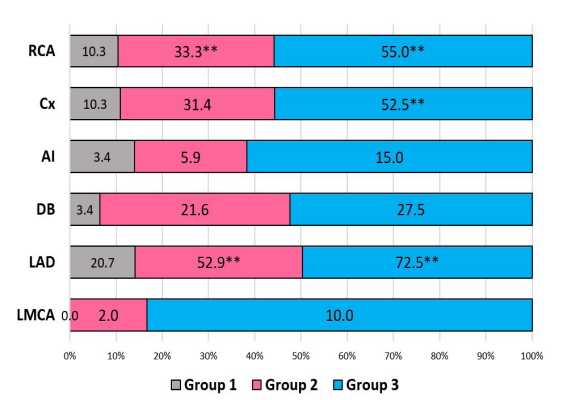
Figure 1: Comparative analysis of the incidence of major coronary artery lesions.
Notes: Data are presented as percentages; LMCA – left main coronary artery; LAD – anterior interventricular branch; DB – diagonal branch; AI – intermedia artery; Cx– circumflex artery; RCA – right coronary artery; ** – significant differences with Group 1 (control) at p<0.0001
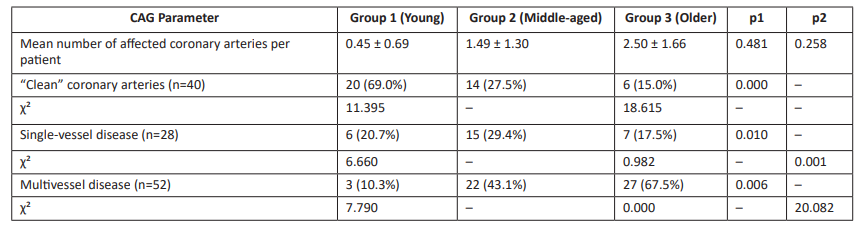
Table 1: Coronary Artery Involvement by Age Group
Coronary artery stenosis also exhibited age-related patterns. In younger patients (Group 1), the most pronounced stenoses were observed in the RCA and circumflex artery (Cx) territories, reaching 99.7% and 98.7%, respectively. In older patients, the mean stenosis across different coronary territories was 51.0 ± 32.8% for the left main coronary artery (LMCA), reflecting a high degree of atherosclerotic involvement in this age category.
Furthermore, the frequency of coronary artery occlusions was significantly higher in older patients, accounting for 51.6% of all occlusions in the study population. In the intermediate-age group, this proportion was 32.3%, and among younger patients, 16.1% of all occlusions were observed. These data indicate a trend toward more pronounced progression of atherosclerosis with increasing age.
As shown in Table 1, the proportion of “clean” coronary arteries (without significant stenosis) was highest among younger patients (69.0%) and lowest in older patients (15.0%). Multivessel disease was markedly more frequent in older individuals, affecting 67.5% of cases, compared with only 10.3% in younger patients. These findings confirm the higher burden of multivessel coronary involvement in the elderly population. Table 1.
Overall, age-related differences in clinical and coronary angiographic characteristics demonstrate a trend toward increased disease severity with advancing age. Younger patients more frequently presented with acute forms of ischemic heart disease (IHD), often accompanied by arrhythmias and microvascular angina. In contrast, older patients exhibited more pronounced chronic IHD and extensive multivessel coronary involvement, associated with a higher risk of coronary occlusions and arterial calcification.