Traumatic Human Bite Wound on the Lower Lip: A Case Report
Dr Gabriel Mpundu1,3; Dr Emmanuel Muwowo1; Dr Mutinta Syalucha1; Mr Crecious Phiri2; Mr John Soko2
¹Levy Mwanawasa University Teaching Hospital, Oral Health and Maxillofacial Department
²Levy Mwanawasa Medical University, Public Health Department
³Levy Mwanawasa Medical University, School of Medical and Clinical Sciences
*Corresponding author
Gabriel Mpundu, Levy Mwanawasa University Teaching Hospital, Oral Health and Maxillofacial Department
Email: gmpundu3@gmail.com
DOI: 10.55920/JCRMHS.2025.12.001552
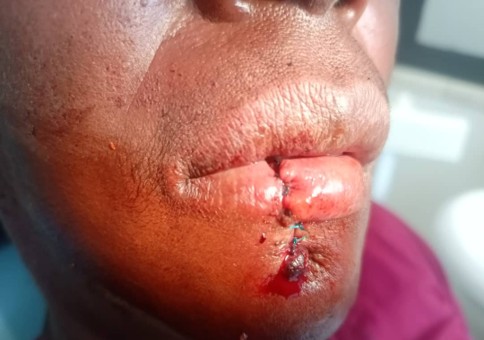
Figure 1: Pre Operative
Thoracic CT scan revealed the wide spread emphysema of the right buccal region, and the cervical spaces extending to the anterior and posterior mediastinum (Fig. 2).
Figure 2: Post Operative
Conservative treatment included nonsteroidal anti-inflammatory drugs and preventive antibiotic therapy with ceftriaxone. The patient was prescribed bed rest. After nine days the swelling resolved, physical examination and control chest X-ray were normal. The patient was discharged and maintained follow-up in as a stomatology outpatient for extraction of teeth.
Figure 3: Post Operative
Postoperative management consisted of oral analgesics (ibuprofen 400 mg every 8 hours for 5 days) and broad-spectrum antibiotic coverage (amoxicillin 500 mg every 8 hours for 5 days combined with metronidazole 500 mg every 8 hours for 5 days). A stat dose of tetanus toxoid (0.5 mg) was also administered. To minimize cicatrization-related complications, silk sutures were removed after 2 weeks.
Although wound cultures were not performed due to limited resources, the patient was closely monitored for signs of infection. In addition, HIV screening and counselling were offered, and the patient was informed about the potential risk of viral transmission associated with human bite injuries.
At her 6-month follow-up, the patient had healed well, with good aesthetic and functional outcomes. She was able to speak, eat, and maintain lip competence without difficulty, and scarring was minimal.
From a public health perspective, this case underscores the burden of interpersonal violence as a cause of traumatic human bites in Zambia. Such injuries not only carry risks of infection and disfigurement but also highlight the importance of violence prevention, community education, and timely access to oral surgical care.
This case demonstrates that a simple surgical procedure, if performed promptly and appropriately, can result in excellent functional and aesthetic outcomes for human bite injuries of the lip.
Table 1: Lackmann’s classification of facial bite injuries