Pemphigus Vulgaris: A Case Report
Amna Jarouf, Nemat Alsaghir, Hanaa Almsokar, Kinda Alshawa
Department of Dermatology, Hospital of Dermatology and Venereology, Damascus.
*Corresponding author
Amna Jarouf, Department of Dermatology, Hospital of Dermatology and Venereology, Damascus.
Email: jarouf4.amna@damascusuniversity.edu.sy
kinda.alshawa@damascus university.edu.sy
Nemat.alsaghir@damascusuniversity.edu.sy
DOI: 10.55920/JCRMHS.2025.12.001520
Abstract
Pemphigus vulgaris (PV) is a rare, potentially life-threatening autoimmune blistering disorder characterized by IgG autoantibodies against desmoglein 3 and, in some cases, desmoglein 1, leading to intraepidermal acantholysis and blister formation. A rare clinical variant, pemphigus vegetans, accounts for 1–2% of pemphigus cases and presents with papillomatous, vegetative plaques primarily in intertriginous regions. We report the case of a 55-year-old woman with no significant medical history who presented with progressive lip swelling, painful fissures, and vegetative plaques. Clinical examination revealed oral mucosal involvement and erythematous plaques on the trunk and lower extremities. Histopathology confirmed features consistent with vegetative pemphigus. The patient responded favorably to systemic corticosteroids and adjunctive therapies, with marked improvement observed within weeks. This case highlights the importance of recognizing atypical variants of PV for timely diagnosis and effective management.
Introduction
Pemphigus vulgaris (PV) is a rare, potentially life-threatening autoimmune blistering disorder characterized by the formation of flaccid bullae and erosions on the skin and mucous membranes. The pathogenesis involves IgG autoantibodies targeting desmoglein 3 and, in some cases, desmoglein 1—cadherin-type cell adhesion molecules integral to desmosomal integrity in stratified squamous epithelia. This antibody-mediated disruption leads to acantholysis, resulting in intraepidermal blistering. Clinically, PV often begins with painful oral erosions that may precede cutaneous involvement by several months. Without timely immunosuppressive treatment, PV can progress rapidly and was historically associated with high mortality rates; however, the advent of systemic corticosteroids and biologic agents such as rituximab has significantly improved prognosis [1,2].
A rare clinical variant, pemphigus vegetans, accounts for approximately 1–2% of pemphigus cases and is characterized by vegetative, papillomatous plaques, typically occurring in intertriginous areas like the groin, axillae, and perioral region. Two subtypes are recognized: the Neumann type, which evolves from bullous lesions and follows a more aggressive course, and the Hallopeau type, which arises from pustular lesions and tends to be more indolent. Despite clinical differences, both subtypes share the pathogenic mechanism of autoantibodies against desmoglein 1 and 3. Management includes systemic corticosteroids, with additional therapies such as retinoids considered for recalcitrant disease [3,4].
Case Report
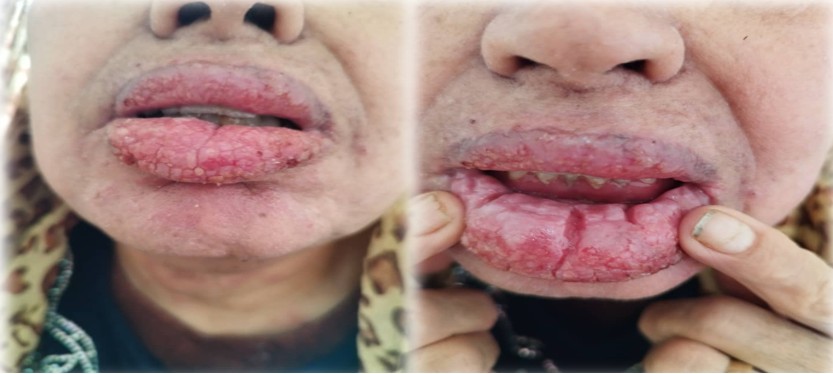
A 55-year-old female patient, a non-smoker, non-alcoholic, with no medical, drug, allergy, or surgical history, presented to the clinic with complaints of swelling of the upper and lower lips. The patient's history began approximately a year and a half ago. The swelling gradually increased, with fissures extending into the mouth and pain on pressure [Figure 1].
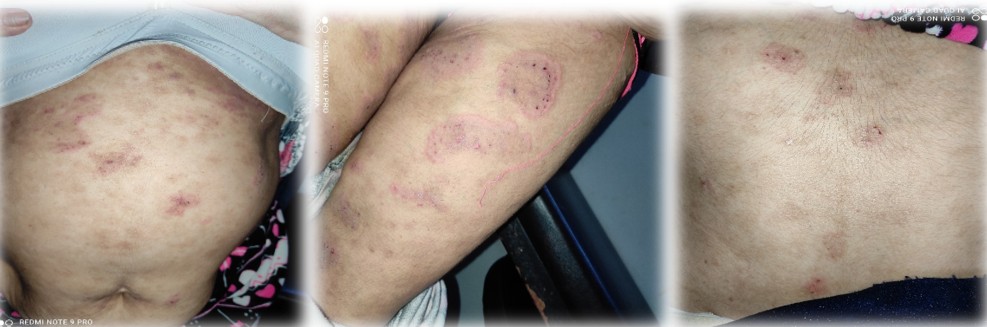
Clinical examination revealed swelling of the upper and lower lips with fissures extending into the oral and buccal mucosa, as well as vegetative plaques on the lips and some scabs and erosions [Figure 2], and annular erythematous plaques on the trunk and lower extremities [Figure 3].
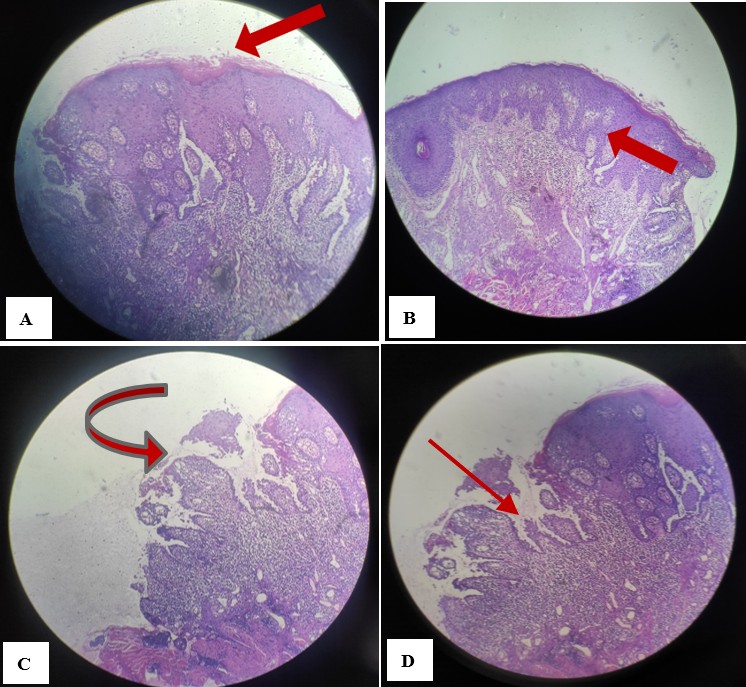
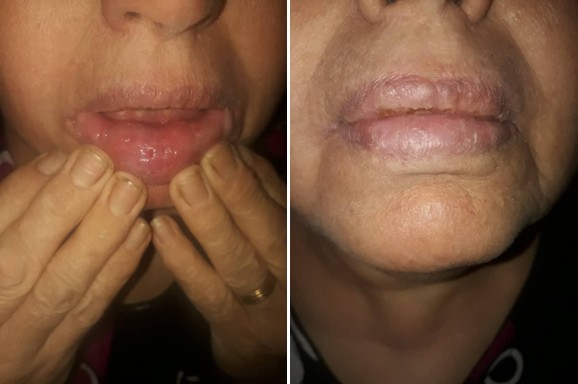
The patient's biopsy results showed hyperkeratosis, acanthosis, gravestone sign, and lymphocytic and plasma cell infiltration [Figure 4]. Laboratory tests were within the normal range. Final diagnosis: vegetative pemphigus (a rare form of pemphigus vulgaris). Treatment: Prednisolone 1 mg/kg/day, topical steroids to treat oral lesions, nystatin, calcium, and vitamin D to prevent osteoporosis. Treatment results appear within two weeks of initiation [Figure 5] and after several months [Figure 6].
Figure 1 :Swelling with cracks extending into the mouth.
Figure 2 : Vegetative plaques on the lips, some scabs and erosions
Figure 3 : Annular erythematous plaques on the trunk and lower extremities
Figure 4 : Tissue biopsy result. (A) Hyperkeratosis, (B) Acanthosis, (C) Epidermal Bulla, (D) Tombstone Mark
Figure 5: Treatment result after two weeks
Figure 6: Treatment result after few months
Discussion
This case highlights a diagnostically and clinically significant presentation of “pemphigus vegetans”, a rare and localized variant of “pemphigus vulgaris (PV)”, characterized by its “vegetative mucocutaneous lesions”. Although histopathological examination of the patient’s biopsy demonstrated features classically associated with PV such as “suprabasal acantholysis, the "row of tombstones" appearance, hyperkeratosis, and acanthosis” the “distinctive clinical presentation”, with “vegetative plaques on the lips, erosions, and annular erythematous plaques on the trunk and lower limbs”, is more consistent with “pemphigus vegetans”.
“Pemphigus vegetans is a well-recognized clinical variant of PV”, and while it shares the same underlying autoimmune pathophysiology predominantly the presence of autoantibodies against desmoglein 3 it is distinguished by its localized, exophytic lesions and less aggressive course. The “plasma cell-rich infiltrate and pseudoepitheliomatous hyperplasia” seen on biopsy further support this diagnosis and reflect the chronic, reactive epithelial hyperplasia typical of vegetans-type lesions.
Treatment with “systemic corticosteroids (prednisolone 1 mg/kg/day)” resulted in a “rapid and sustained clinical response”, with visible improvement in mucocutaneous lesions noted within two weeks and further resolution seen over the following months. This favorable outcome is in agreement with Mimouni et al. (2006) [5], who emphasized that pemphigus vegetans, while rare, typically responds well to “first-line corticosteroid therapy”, with early initiation correlating with faster disease control.
Furthermore, Ahmed and Dahl (2003) [6] underscore the importance of early systemic corticosteroids to prevent complications and achieve remission in PV variants. While some pemphigus vegetans cases reported in the literature require adjunctive immunosuppressive agents such as “azathioprine” or “mycophenolate mofetil”, especially in extensive or recalcitrant disease (as noted by Kirtschig et al., 2010) [7], our patient exhibited “a robust response to corticosteroids alone”. This suggests either a more localized disease course or effective early intervention.
In addition to systemic therapy, the patient was prescribed “topical corticosteroids” for oral lesions and “nystatin” for antifungal prophylaxis. To mitigate corticosteroid-associated risks, “calcium and vitamin D supplementation” were included, aligning with current best practices in long-term glucocorticoid management.
Finally, comparison with the retrospective study by Shamim et al. (2008) [8], involving 71 cases of oral PV, reveals that the “mucosal-dominant pattern” and the “early steroid responsiveness” seen in our case are in keeping with the clinical behavior of early or localized pemphigus variants. However, the “vegetative and hypertrophic mucosal features”, coupled with histopathological evidence of epithelial hyperplasia and inflammatory infiltrate, provide strong support for “pemphigus vegetans” as the more accurate clinical diagnosis—despite biopsy overlap with classic PV.
This case underscores the importance of integrating “clinical morphology”, “histopathological features”, and “therapeutic response” when differentiating among pemphigus variants. Accurate subclassification has implications not only for prognosis but also for the optimization of treatment strategies.
Conclusion
This case highlights presentation of pemphigus vulgaris in a 55-year-old woman who developed painful lip swelling, oral fissures, and vegetative plaques on the skin and mucous membranes. Histopathology confirmed the diagnosis of pemphigus vegetans, a rare clinical variant. Importantly, this case emphasizes that pemphigus vulgaris may initially manifest not only as mucous blisters and erosions but also as vegetative plaques, particularly in atypical or early presentations. Recognizing these patterns is crucial for early diagnosis and timely treatment, which can significantly improve patient outcomes.
Declaration of competing interest: All the authors declared that they have no conflicts of interest.
Consent: Written patient consent was obtained before reporting this case and before using any of his medical information or pictures.
Ethical approval: This study has been approved by the ethical committee of Damascus University.
Formatting of funding sources: This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Availability of data and materials: All data are available from the corresponding author on reasonable request.
Funding: This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
References
- Amber KT, Hertl M. "An assessment of treatment history and its impact on disease outcomes in pemphigus vulgaris." Br J Dermatol. 2018.
- Schmidt E, Zillikens D. "Pemphigus and bullous pemphigoid." Lancet. 2013.
- Pruitt DL, et al. "Pemphigus vegetans: A rare variant of pemphigus vulgaris." J Multidiscip Healthc. 2019.
- Orphanet. "Pemphigus vegetans – rare disease information." Accessed 2024.
- https://www.sciencedirect.com/science/article/abs/pii/S0151963806776116
- Kljuic A, Bazzi H, Sundberg JP, Martinez-Mir A, O'Shaughnessy R, Mahoney MG, Levy M, Montagutelli X, Ahmad W, Aita VM, Gordon D, Uitto J, Whiting D, Ott J, Fischer S, Gilliam TC, Jahoda CA, Morris RJ, Panteleyev AA, Nguyen VT, Christiano AM. Desmoglein 4 in hair follicle differentiation and epidermal adhesion: evidence from inherited hypotrichosis and acquired pemphigus vulgaris. Cell. 2003 Apr 18;113(2):249-60. doi: 10.1016/s0092-8674(03)00273-3.
- May K, Bryant A, Dickinson HO, Kehoe S, Morrison J. Lymphadenectomy for the management of endometrial cancer. Cochrane Database Syst Rev. 2010 Jan 20;(1):CD007585. doi: 10.1002/14651858.CD007585.pub2. Update in: Cochrane Database Syst Rev. 2015 Sep 21;(9):CD007585. 10.1002/14651858.CD007585.pub3. PMID: 20091639; PMCID: PMC4171003.
- Shamim T, Varghese VI, Shameena PM, Sudha S. Pemphigus vulgaris in oral cavity: clinical analysis of 71 cases. Med Oral Patol Oral Cir Bucal. 2008 Oct 1;13(10):E622-6.