Study of Thyroid and Lipid Profile in Perimenopausal Women to Find Out Relation Between Them
Dr. Khom bahadur Chaudhary*, MS Nilam chaudhary
Infectious and Communicable Disease Hospital, Rapti Academy Of Health Sciences Pokhara, Nepal.
*Corresponding author
MS Nilam Chaudhary, Infectious and Communicable Disease Hospital, rapti Academy Of Health Sciences Pokhara, Nepal
DOI: 10.55920/JCRMHS.2025.11.001499
Abstract
Introduction: Perimenopausal women are at high risk of several health problems including thyroid disorders and dyslipidemia. But still many of them are undiagnosed in routine health checkup and women are at high risk of morbidity and mortality. Thus the study of thyroid and lipid profile among perimenopausal women is very important and such study are very much limited.
Methods: This is a single-centered, analytical, cross-sectional, observational study. This is carried out among the perimenopausal female patients, who presented to General Health Checkup in General Practice OPD of Tribhuvan University Teaching Hospital. Data collection was started after ethical clearance from Institutional Review Committee. The data was analyzed through SPSS version 22 for data analysis. Data was analyzed by fisher exact test and Chi Square test.
Results: Total 96 patients who fulfilled inclusion criteria were studied. Mean age of patients of our study was 48.3 yrs. (SD 4.6), Mean pulse rate was 76.2(8.7) b/m, mean weight was 56.1(7.8) yrs., mean BMI was 22.9(4.1) kg/m2. The mean of TG, TC, LDL, HDL were 1.3(0.5), 4.7(1.2), 2.9(1.3), 1.6(0.8) mmol/L respectively. The mean of T3, T4 and TSH were 6.7(1.9), 16.5(5.7), 3.6(2.3) respectively. In this study euthyroid were 72.9 %, hyperthyroidism 8.3 %, overt hypothyroidism 3.1 % and subclinical hypothyroidism were 15.6%. In this study, 53.3% of patients had high cholesterol among subclinical hypothyroidism and 33.3% had high cholesterol among overt hypothyroidism. 33.3% of patients had high triglycerides level among overt hypothyroidism and 26.7% had high triglycerides among subclinical hypothyroidism. In this study, 40.0% had very high LDL level among subclinical hypothyroidism and 33.3% had very high LDL among overt hypothyroidism. 53.3% had poor HDL level among subclinical hypothyroidism and 33.3% of overt hypothyroidism had poor HDL level. Also 42.9% of euthyroid patients had best HDL level.
Conclusion: In perimenopause women, there is increase in mean TC, TGs, LDL cholesterol, and decrease in HDL cholesterol among patients with thyroid disorder mostly subclinical hypothyroidism. Thyroid disorder and dyslipidemia were closely associated among perimenopausal women.
Keywords: Perimenopause, HDL, LDL, total Cholesterol, Triglycerides, Hypothyroidism, Dyslipidemia
Introduction
Perimenopause is an ill-defined time that surrounds the final years of a woman's reproductive life. It begins with the first onset of menstrual irregularity and ends after 1 year of amenorrhea has occurred, thereby defining the final menstrual period (FMP). There are two stages to the perimenopause or menopausal transition: the early transition, where cycles are mostly regular, with relatively few interruptions, and the late transition, where amenorrhea becomes more prolonged and lasts for at least 60 days, up to the FMP. Several worldwide cohorts have defined the natural history of the menopausal transition in sufficient detail such that these stages have been broken down and linked to specific hormonal events, which in turn are linked to symptoms. (1)
When the number of ovarian follicles diminishes, the release of the ovarian hormones estrogen and progesterone decreases, resulting in menopause. Hormonal changes after menopause, such as lower plasma estrogen levels and higher Luteinizing Hormone (LH) and Follicle Stimulating Hormone (FSH) levels, have a significant impact on lipid and lipoprotein metabolism in the blood. Estrogen levels have an impact on lipid metabolism.
Serum lipids and lipoproteins have been shown to vary during menopause in previous studies. Low estrogen levels in the blood and a major increase in LH and FSH levels have a significant impact on plasma lipid and lipoprotein metabolism, as do hormonal changes associated with menopause, such as estrogen, progesterone, and progesterone. (2). Estrogen levels in the body have an impact on lipid metabolism.
A shift in blood lipid profile is connected to menopause. Hypothyroidism and perimenopause share certain symptoms. Women in their forties and fifties are likewise more likely to have hypothyroidism. Around this time, women are going through menopause. In hypothyroid women, estrogen raises the level of thyroxine binding globulin and the need for thyroid hormone. The gonadal axis and thyroid function are linked during a woman's reproductive phase. Thyroid hormones stimulate the production of sex hormone binding globulin, testosterone, and androstenedione, lower estradiol and androgen clearance, and improve the conversion of androgens to estrone, all of which have an indirect effect on reproductive function. Thyroid hormone receptors mediate the direct effects at the oocyte level. Thyroid hormones and follicle stimulating hormone work together to make progesterone in granulosa cells via follicle stimulating hormone receptors. (3).
Methods
Study Design and Setting
This was a single-center, observational cross-sectional study done in female Patients of perimenopausal age group, who presented General Practice OPD for General health checkup, in Tribhuvan University Teaching Hospital. Duration of study was 3 months from September 2021 to November 2021. The ethical approval was approved by Institutional Review Committee of Institute of Medicine.
Inclusion and Exclusion criteria:
Apparently healthy women aged between 40 and 55 years were included in the study. Their thyroid profile and fasting lipid profile were sent and analyzed.
Sample size for the study was calculated by using following formula:
Sample size= Z (1-α) 2 p (1-p)/d2
Where, Z1-α/2 = standard normal variate, 1.96 for 10% type I error
p=expected proportion in population =50% (1)
d= absolute error or precision= 0.1, 10% type I error
Using the above information, a sample size of 96 was estimated at a 95% level of confidence and a precision of 10%.
Consent was taken for participation after a brief introduction and highlighting the study to the patient and accompanying relatives. The patients were screened for study by filling the proforma. Potential inclusion and exclusion criteria were reviewed. Patients who met the inclusion criteria and were enrolled in the study. All necessary clinical examinations was done. The patient were asked for Thyroid profile test(T3,T4 and TSH) on same day and were counselled to follow up in the next morning in a fasting state to give a blood sample for fasting lipid profile. The sample were sent to the laboratory. In Laboratory serum samples were separated for the analysis of Total Cholesterol (TC), Triglycerides (TGs), High-Density Lipoprotein Cholesterol (HDL-C), and Low-Density Lipoprotein Cholesterol (LDL-C). Total cholesterol (TC) was measured using established enzymatic methods of Allain et al. TGs was isolated enzymatically by glycerol-3-phosphate oxidase - phenol+ method as described by Schettler et al. HDL-C direct was isolated by enzyme selective protection method of Williams et al. LDL was calculated using the Friedewald formula: which is valid till TGs level 400 mg/dl.
LDL-C = TC - (HDL-C + TGs/5) when all in mg/dl
The report was tracked and recorded.
After completion of the data collection, data were entered using Microsoft Excel 2007 and later on IBM SPSS Statistics Data Editor Version 16 and analyzed by appropriate statistical tools. Categorical data were expressed as frequencies and corresponding percentages; parametric data were expressed as mean (SD) and compared fisher exact test and chi square test.
Results
96 cases were included in the study.
In our study maximum patients were of age group >= 50 yrs. with 47.9 %.
In our study, we saw Brahmins were maximum with 29.2 %, followed by Chhetri. Minimum were Muslims with 3.1 %.
Among 96 patients studied in our study, we found diabetes among 25 patients and hypertension among 26 patients.
We saw normal cholesterol level in 67.7% of study sample followed by borderline high cholesterol of 19.8% and High cholesterol among 12.5%.
In our study 80.2% of study samples had normal triglycerides level, 13.5% had borderline high, 6.2% had high triglycerides level.
In our study 77.1% had normal LDL level, 15.6% had high LDL level followed by 7.3% of very high LDL level.
In our study, 28.1% had poor HDL level, 33.3% had better HDL level and 38.5% had best HDL level.
In our study, 4.2% had decreased T3 level and 8.3% had high T3 level whereas 87.5% had normal T3 level.
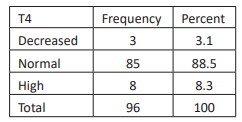
In our study sample, 3.1% had decreased T4 level and 8.3% had high T4 level whereas 88.5% had normal T4 level.
In our study, 8.3% had decreased TSH level and 18.8 % had high TSH level whereas 72.9% had normal TSH level
In our study, 70 patients were euthyroid and 8 patients had hyperthyroidism followed by 3 patient’s overt hypothyroidism and 15 had subclinical hypothyroidism.
Table 1: Age Composition, n= 96
Table 2: Ethnicity distribution, n= 96
Table 3: Cholesterol level among study samples, n=96
Table 4: Triglycerides level among study samples, n=96
Table 5: Low density lipoprotein level among study samples, n=96
Table 6: High density lipoprotein level among study samples,
Table 7: Free T3 level among study samples, n=96
Table 8: Free T4 level among study samples, n=96
Table 9: TSH level among study samples, n=96
Table 10: Thyroid profile and their interpretation
Figure 1: Hypertension and Diabetes among study sample, n=96
Table 11: Thyroid profile and cholesterol level
Table 12: Thyroid Profile and Triglycerides Level
Table 13: Thyroid profile and LDL level
Table 14: Thyroid profile and HDL level
Figure 2: Thyroid profile among study samples
In our study, we saw 53.3% of patients had high cholesterol among subclinical hypothyroidism and 33.3% had high cholesterol among overt hypothyroidism.
In our study, 33.3% of patients had high triglycerides level among overt hypothyroidism and 26.7% had high triglycerides among subclinical hypothyroidism.
In our study, 40.0% had very high LDL level among subclinical hypothyroidism and 33.3% had very high LDL among overt hypothyroidism.
In our study, 53.3% had poor HDL level among subclinical hypothyroidism and 33.3% of overt hypothyroidism had poor HDL level. Also 42.9% of euthyroid patients had best HDL level.
Discussion
In our study, the minimum age of the study population was 40 years and the maximum age was 55 years with a mean age of 48.3(SD 4.6) years. Among the 96 perimenopausal women, maximum ethnic group were from Brahmin (29.2 %) followed by Chhetri (27.1%). The mean BMI was 22.9 kg/m2.
Highest numbers of patients were from age group > 50 yrs. (47.9 %). The 26% of patients had diabetic history and 27.1 % of patient gave history of hypertension. 21.9 % of patient gave alcohol consumption history and 16.7 % of patients gave smoking history.
In our study 80.2% of study samples had normal triglycerides level, 13.5% had borderline high, 6.2% had high triglycerides level. 77.1% had normal LDL level, 15.6% had high LDL level followed by 7.3% of very high LDL level. Also 28.1% had poor HDL level, 33.3% had better HDL level and 38.5% had best HDL level.
Similarly we found that 4.2% had low T3 level and 8.3% had high T3 level whereas 87.5% had normal T3 level. In our study sample 3.1% had decreased T4 level and 8.3% had high T4 level whereas 88.5% had normal T4 level. In our study, 8.3% had decreased TSH level and 18.8 % had high TSH level whereas 72.9% had normal TSH level. 72.9 % patients were euthyroid and 8.3 % patients had hyperthyroidism followed by 3.1% patient’s overt hypothyroidism and 15.6 % had subclinical hypothyroidism. This was similar to study by Bordoloi et al. which showed prevalence of hypothyroidism was found to be 8.2% in premenopausal and 12.7% in postmenopausal women(4)
In our study, among the perimenopausal women group (N= 96), mean TC was 4.7 mmol/L (183.3 mg/dl), TGs was 1.3 mmol/L (115.7mg/dl). Similarly, HDL was 1.6 mmol/L (62.4 mg/dl), LDL was found to 2.9 mmol/L (113.1 mg/dl). We observed a significant increase in serum Total Cholesterol (TC), Triglycerides (TGs), LDL-cholesterol, and VLDL cholesterol levels in perimenopausal women which is similar to a study done by Jenson et al 1998(6), CS et al. 2015 (5) Kilim et al. 2013 (7), Shenoy et al. 2015 (8). Similarly study by Stevenson et al. 1993 (9) found Postmenopausal women had significantly higher concentrations of total cholesterol (p < 0.001), triglycerides (p < 0.005), LDL cholesterol (p < 0.001). Study on the IRACUS group by Aloysilo et al. found higher mean total cholesterol and LDL cholesterol. The study by Igweh et al. (10) also finds a statically significant increase in LDL and VLDL but an increase in TGs which were nonsignificant statically. Similar study by Yeasmin et al. 2019 (11) found statically significant increase in mean TC and TGs level in postmenopausal group than premenopausal group. Result similar to study by Perers et al. which shows significant change for Total Cholesterol and LDL-Cholesterol but not significant (p > 0.05) increase for HDL-C, TGs.
We observed an increase in HDL cholesterol level in the perimenopausal group which is statically significant (p<0.05), which is similar to the study by Pardhe et al 2017, but result from Jensen et al. 1989 (6), Igweh et al. 2005 (10), kilim et al. 2013 (7) CS et al. 2015 (5) Stevenson et al, show a statically significant decrease in the post-menopausal group. A similar result from Shenoy et al. 2015 (8) shows a decrease in mean HDL which is not statically significant. A study by Derby et al. 2009 shows an increase in mean HDL in early menopause as compared to premenopausal and which decreases compared to the premenopausal level in late menopause. (13)
Most of the study result including our study shows the increase in lipid parameter among perimenopausal women with an exception for HDL. For HDL. The result from our and few study show increase HDL cholesterol level among post-menopausal women which is statically significant whereas some article shows a decrease in HDL level.
Conclusion
With increasing age in perimenopause women, there is increase in mean TC, TGs, LDL cholesterol, and decrease in HDL cholesterol among patients with thyroid disorder mostly subclinical hypothyroidism. Thyroid disorder and dyslipidemia were closely associated among perimenopausal women.
Declaration
Acknowledgement: We express our sincere thanks to Department of General Practice and Emergency Medicine and of Tribhuvan University Teaching Hospital, Kathmandu for giving us the opportunity to conduct this study in the premises. Special acknowledgment to all who were directly or indirectly involved in this research for their valuable help.
Conflict of interest: None
Funding: None
Ethical clearance: Ethical clearance was obtained from IRC IOM TUTH, before conducting this study and a written consent was also taken from department of General Practice and Emergency Medicine, Tribhuvan University Teaching Hospital before data collection.
Consent for study: Written informed consent was taken from each participants
Consent for publication: It was taken from researchers as mentioned in authorship declaration form.
References
- Linton MF, Yancey PG, Davies SS, Jerome WG, Linton EF, Song WL, et al. The role of lipids and lipoproteins in atherosclerosis. : MDText. com, Inc.; 2019.
- Phan BAP, Toth PP. Dyslipidemia in women: etiology and management. Int J Womens Health. 2014;6:185-94.
- Witteman JC, Grobbee DE, Kok FJ, Hofman A, Valkenburg HA. Increased risk of atherosclerosis in women after the menopause. BMJ. 1989;298(6674):642-4.
- Bordoloi G, Jahan W. A study of thyroid function in premenopausal and postmenopausal women of Dibrugarh town, Assam, India. Int J Res Med Sci. 2018;6:3015–9. doi: 10.18203/2320-6012.ijrms20183636. [DOI] [Google Scholar]
- Cs A-O, Pe O, Pi O, S N, G O-U, Okorocha A, et al. Coronary Artery Disease and Menopause: A Consequence of Adverse Lipid Changes. IOSR Journal of Dental and Medical Sciences. 2015;14:7-11
- Jensen J, Nilas L, Christiansen C. Influence of menopause on serum lipids and lipoproteins. Maturitas. 1990;12(4):321-31.
- Reddy Kilim S, Chandala SR. A comparative study of lipid profile and oestradiol in pre- and post-menopausal women. J Clin Diagn Res. 2013;7(8):1596-8.
- Shenoy R, Vernekar PJIJoSS. Fasting lipid profile in pre-and postmenopausal women: a prospective study. 2015;3(9):116-9.
- Anagnostis P, Stevenson JC, Crook D, Johnston DG, Godsland IFJM. Effects of menopause, gender and age on lipids and high-density lipoprotein cholesterol subfractions. 2015;81(1):62-8.
- Igweh JC, Nwagha IU, Okaro JM. The effects of menopause on the serum lipid profile of normal females of South East Nigeria. Nigerian journal of physiological sciences : official publication of the Physiological Society of Nigeria. 2005;20(1-2):48-53.
- Yeasmin, N., Akhter, Q. S., Mahmuda, S., Nahar, S., Abira, M., Rahman, F., … Yeasmin, S. (2019). Association of Serum Triglycerides and Total Cholesterol levels with Hypertension in Adult Female. Bangladesh Critical Care Journal, 7(1), 35–39. https://doi.org/10.3329/bccj.v7i1.40763
- Shenoy R, Vernekar PJIJoSS. Fasting lipid profile in pre-and postmenopausal women: a prospective study. 2015;3(9):116-9.
- Derby CA, Crawford SL, Pasternak RC, Sowers M, Sternfeld B, Matthews KA. Lipid changes during the menopause transition in relation to age and weight: the Study of Women's Health Across the Nation. American journal of epidemiology. 2009;169(11):1352-61.