Treatment of Toe-Tip Amputation in Children. Presentation of a New Technique with Occlusive Dressing and Review of the Literature
Johannes Wirmer1*, Jurek Schulz2
¹Department of Pediatric Surgery, Sana Klinikum Offenbach, Germany.
²Department of Pediatric Surgery, Universitätsklinikum Dresden, Fetscherstrasse 74, 01307 Dresden, Germany
*Corresponding author
Johannes Wirmer, Department of Pediatric Surgery, Sana Klinikum Offenbach, Germany.
DOI: 10.55920/JCRMHS.2025.11.001495
In the following outpatient controls, the distal part of the toe presented increasingly livid, until it was fully necrotic, so that 17 days after the trauma it was removed. The removal was possible without anesthesia and absolutely pain free, proving the complete necrosis.
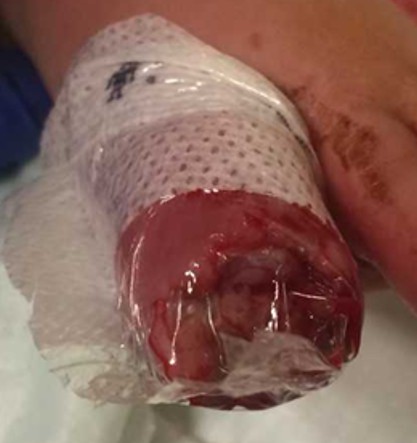
Subsequently, there was an open defect at the level of the basal nail wall with exposed bone of the remaining distal phalanx, which was treated with a semi-occlusive bandage, using Tegaderm TM Film transparent dressing (see Fig. 2-4).
The patient was then called back for a weekly dressing change. Already two weeks after the start of the occlusive treatment, the previously exposed bone was covered with granulation tissue, with the skin defect still presenting (Fig. 5 + 6). In the absence of discomfort, the foot was released for careful loading according to the child's measures. The follwoing controls showed increasing regeneration of the tip with simultaneous epithelialization (see Fig. 7), so that the semi-occlusive treatment could be ended after 8 weeks.
The final check-up 4 months after the trauma showed a non-irritated, slightly shortened toe with an irregularly growing toenail (see Fig. 8). There was no discomfort, the patient and the parents were very content.