¹First-degree specialist in general medicine and gynecology and obstetrics. Instructor professor. Dr. Mario Muñoz Monroy Hospital, Colón, Cuba.
²First-degree specialist in gynecology and obstetrics. Instructor professor. Piti Fajardo Hospital,Cuba.
Dr. Deivys Rodríguez Navarro, FirstDegree Specialist in General Medicine and Gynecology and Obstetrics. Instructor Professor. Dr. Mario Muñoz Monroy Hospital, Colón, Cuba.
Abstract
Introduction: Pregnancy and childbirth care practices vary widely between countries, institutions and the different teams in charge of obstetric care: in this context with such diverse practices, evidence-based clinical practice allows the actions of professionals to those in charge of obstetric care is based on the best available evidence where cervical ripening/induction of labor is indicated when there is some maternal or fetal risk that, if the pregnancy continues, is greater than the risk of birth early or before the spontaneous onset of labor. Induction of labor is a relatively common procedure. In the United States the prevalence of induction is 23.3%, while in the United Kingdom it is 20% and in Canada 21%.
Methodology: A descriptive, longitudinal study was carried out, which included patients with a healed uterus of more than six months in first trimester pregnancies and more than two years in second and third trimester pregnancies, which due to medical indication required termination of pregnancy, without contraindications for it, and where the placement of the endocervical balloon catheter was used as the method of choice. Where the main indication was the death of the product of conception.
Conclusions: It is evident that although the pharmacological methods for cervical ripening and induction of labor are effective and with a minimum of maternal-fetal complications, the methodology and procedures used since the most remote times in the history of obstetrics continue to have their precise indications and usefulness in special cases, thus achieving 92 % effectiveness in triggering labor.
Keywords: Endocervical balloon, induction of labor.
Cervical ripening is the process that involves changes in shape, position, consistency, and endocervical canal, which are essential for vaginal delivery (1). This process can be accelerated using various methods to improve cervical conditions for induction.
Induction of labor, one of the most widely used techniques in obstetrics, is the procedure aimed at triggering uterine contractions in an attempt to induce vaginal delivery when there is an indication to terminate the pregnancy and this does not occur spontaneously (2).
Induction of labor is considered indicated when the benefits of terminating the pregnancy for the mother and fetus outweigh those of allowing the pregnancy to continue. These situations are listed below:
– Maternal pathology: hypertensive disease of pregnancy, neuropathies, heart disease, chronic obstructive pulmonary disease, diabetes, neoplasia, etc.
– Obstetric indications: prolonged pregnancy, premature rupture of membranes, chorioamnionitis, others.
– Indicaciones fetales: isoinmunización Rh, crecimiento intrauterino retardado, feto muerto, anomalías congénitas.
Cervical conditions in labor induction: The success of an induction depends on the initial cervical conditions (2). In 1964, Bishop devised a systematic method for assessing cervical conditions. This system assesses, through vaginal examination, cervical characteristics (dilation, shortening, consistency, position in the vaginal vault, and height of the presentation in the pelvis) with a score from 0 to 3 (Table 1). The sum of the scores predicts the success of labor induction, which, according to the Spanish Society of Obstetrics and Gynecology (SEGO), is:
- Bishop >7, 95% success rate.
- Bishop 4-6, 80-85% success rate.
- Bishop <3, 50% success rate.
When the Bishop score is six or less, cervical ripening should be performed prior to induction (3). The higher the ripening achieved, the higher the success rate, with a Bishop score of seven or greater being taken as the reference value.
Contraindications to cervical ripening are those situations that contraindicate induction, such as:
- Occlusive placenta previa.
- Transverse or oblique position.
- Previous uterine surgery with entry into the cavity.
- Classic cesarean section or T-section augmentation.
- Demonstrated pelvic-cephalic disproportion.
- Lack of fetal well-being.
- Active genital herpes (due to the risk of fetal infection).
- Invasive cervical carcinoma
Cervical Ripening Methods: The different methods for cervical ripening can be grouped into three broad categories: alternative, mechanical, and pharmacological.
Alternative Methods: It is important to name these methods, not because of their practical importance, but to understand that cervical ripening has been a practice since ancient times, and that the first
Settlers knew that there were situations in which labor had to be induced. Among them, the following stand out:
- Herbs. Evening primrose oil and red raspberry leaves have certain uterotonic and oxytocin-releasing properties (4).
Sexual arousal produces the release of endogenous prostaglandins that act on the cervix. This effect is increased in cases of cervical stimulation and by the presence of prostaglandins in human semen. Orgasm in women also produces the release of prostaglandins (5).
- Acupuncture. Used in China and Japan for over two thousand years, it is based on the stimulation of certain parts of the body using small needles at specific points. In Europe, between 12 and 19% of the population recognizes its use. A variation of this technique is cutaneous electrostimulation. The number of clinical trials is limited, but some have achieved a labor induction rate of 78% (6).
- Nipple stimulation. It results in the release of oxytocin. The problem is that the release is uncontrolled and varies greatly between women. It appears to lack a maturational action in women with unfavorable cervixes (Bishop < 7). The limited number of studies means that the safety of the method has not been fully proven; therefore, it should not be used in high-risk pregnancies (7).
Mechanical Methods
These were the first methods developed and are based on direct dilation of the cervix. Most of them are no longer used in practice, although some are used in special situations (8).
Kelp stems. Kelp is a very common seaweed on our coasts. Once dried and pressed, it forms stems that are inserted into the endocervical canal. It absorbs water from the vaginal mucosa and expands, dilating the endocervical canal. There is a certain risk of uterine perforation, infection, and bleeding.
Hydroscopic dilators, balloon dilators. These are instruments similar to Foley catheters, which are also sometimes used. The catheter is inserted into the endocervix and the balloon at the level of the internal cervical os (ICO). The balloon is expanded with saline solution. This produces direct cervical dilation, as well as the release of oxytocin via the Ferguson reflex. Its complications are similar to those of laminaria stems, except for the risk of perforation. In some women, sudden dilation of the IOC can produce vasovagal reactions that can be severe.
Amniotomy. This causes the rupture of the bonds between the sac and the decidua, which releases prostaglandins. Furthermore, it promotes the descent of the fetal presentation, and the fetal axis will transmit the full force of the contraction to the cervix, producing a more effective contraction. Stimulation of the cervix, in turn, via the Ferguson reflex, will increase the release of oxytocin. Currently, amniotomy is considered a method of induction but not of maturation.
Hamilton maneuver. This involves inserting a finger at the level of the left occipital region (OL), making a 360° movement to detach the lower pole of the sac, thereby achieving the release of prostaglandins. Its risks include accidental rupture of the sac, infection, and bleeding. It causes discomfort during the examination. Detachment of membranes, as a general practice in pregnant women at term, has been associated with a reduction in the duration of pregnancy and in the frequency of pregnancies beyond week 41 (9).
Pharmacological Methods
These are the most commonly used methods today, with prostaglandins being the most common.
- Relaxin. Initially, purified porcine relaxin was used, but the recombinant human form is currently used. The cesarean section rate is 21%, with no reports of hypersystoles with fetal repercussions (10).
- Oxytocin. This is a hormone similar to that secreted by the posterior pituitary gland. Along with amniotomy, it is the most common form of labor induction. Currently, its role in cervical ripening is limited.
- Prostaglandins. This is the most widely used pharmacological method. These are substances derived from arachidonic acid. Prostaglandin receptors are constitutive, unlike the oxytocin receptor, which is induced by gestational age (11).
The increase in prenatal diagnostic methods and improved pregnancy monitoring allow for early detection of maternal and fetal risk factors. This increases the need for safer and more effective cervical ripening methods. It is estimated that the total number of inductions in tertiary care hospitals in Spain reaches 12% of all births (12). In countries such as the United States, the number of inductions is increasing, reaching 18.4%.
FOLEY CATHETER. This involves inserting a thin, soft rubber catheter into the cervix. The catheter has a small balloon at its end, which fills with water, creating a sphere about the size of an almond. This procedure is painless and only slightly uncomfortable. The Foley catheter will produce gentle contractions, often barely perceptible, which will gradually improve cervical health, allowing for another induction method to be continued the following day if this method does not result in labor. This method will allow you to live a “normal life”, walk, eat, shower, etc.
You should notify the staff if you notice that the catheter is "wet." This could mean that the balloon of the Foley catheter could rupture, or that the bag of waters could accidentally break. You should also notify the staff if the catheter comes out on its own without being removed by the appropriate personnel. The Foley catheter is left in place for 24 hours, after which the gynecologist will reassess its use.
It is important to clarify that for many authors in their reviewed studies, having had a prior cesarean section contraindicates the use of this method of labor stimulation. However, a minority of authors consider it a relative contraindication. This is why, given the social and religious customs of the population, Djibouti has a protocol that allows its use, ensuring that a transpelvic birth is performed whenever possible, since multiple cesarean sections would greatly limit the number of children per woman. Always conditioned by correct obstetric monitoring.
Methods: A descriptive, longitudinal study was conducted. Patients with a scarred uterus of more than 6 months in the first trimester and more than 2 years in the second and third trimester were included. Patients who required medical termination of pregnancy, with no contraindications, were medically indicated. The endocervical balloon catheter was the method of choice. The primary indication was death of the product of conception. The sample consisted of 26 patients all with a healed uterus and no contraindications for transpelvic delivery, coinciding with the sample.
Objective: To demonstrate the efficacy and safety of using the Foley balloon catheter as a cervical ripener and labor inducer in patients with previous cesarean sections. Balbala Hospital, 2022-2023.
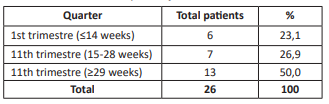
Table 1: Gestational age at which the Foley catheter was inserted. Mohamed Ahmed Issè Hospital, Djibouti. 2022-2023.
Analysis and discussion of the results.
In most of the studies reviewed, the use of any method of labor augmentation and induction, whether mechanical or medical, alone or combined with other methods, is generally employed in pregnancies at or near term, where a specific condition that endangers the survival of the mother, the fetus, or both, necessitates termination of pregnancy. In our study, as previously mentioned, given the social and religious customs of the population, a transpelvic delivery is preferred whenever possible, since multiple cesarean sections would greatly limit the number of children per woman. Therefore, the use of a Foley catheter is a maneuver to stimulate and trigger vaginal labor.
Of the 26 patients in the study sample, 23.6% were in their first trimester, so their diagnosis for termination of pregnancy was the presence of a missed abortion. With only one patient above in the second trimester, and 50% of the total sample in the third trimester, factors that would also favor the success of the technique used.
Pennell, Henderson, Oneil, McChlery, Donety, and Dickinson (2009) conducted a randomized controlled trial comparing the efficacy and user satisfaction of a double-balloon Foley catheter and a single-balloon catheter. The results concluded that induction of labor in nulliparous women with an unfavorable cervix results in high rates of cesarean delivery, and although all methods in this study achieved similar efficacy, the single-balloon catheter offers the best combination of safety and patient comfort (13). Without a doubt, the cervix of a woman who has not had a transpelvic birth does not have the same characteristics as one who has been exposed, once or several times.
to the physiological changes caused by the physical and humoral mechanisms experienced during the effacement and dilation process. Although in our study, this variable did not matter whether it occurred before or after the cesarean section, the reality is that having a vaginal delivery before the cesarean section (55.7%) or after it (30.8%) is a factor favoring the success of catheter placement.
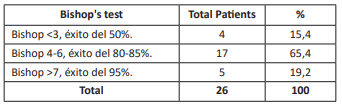
While there is no universally accepted definition for a favorable or unfavorable cervix, higher Bishop scores are associated with a higher likelihood of vaginal delivery, and lower scores with a higher likelihood of cesarean delivery. Therefore, a Bishop score greater than or equal to six will be considered favorable. In cases where the Bishop score is less than or equal to three, it will be considered unfavorable, and a cervical ripening method should be performed prior to delivery. Values of four and five on the Bishop score are considered to be in the gray or intermediate zone. It should be noted that beyond the Bishop score assigned to the patient according to their cervical characteristics at the time of deciding on ripening/induction, there are other characteristics associated with the probability of success of the procedure. These characteristics will help us decide which method to use, especially in cases of Bishop score four and five.
Fortunately, in our sample, only four patients (15.4%) had a Bishop score less than 3,with the majority being in the range of 4 to 6 (65.4%), which admitted them as ideal candidates for the application of the Foley catheter as a method of stimulation and triggering transvaginal labor.
In 2010, Oliveira, Oberst, Leite, Aguemi, Kenj, Zeme, and Sass conducted a randomized clinical trial comparing the efficacy of a Foley catheter with vaginal misoprostol for cervical ripening and labor induction. Activated misoprostol resulted in a higher rate of spontaneous delivery, required less oxytocin use, but was associated with a higher incidence of tachysystole, while the Foley catheter caused more discomfort for the patient. In both studies, there were no differences in the time required to achieve favorable cervical changes to initiate labor, nor in cesarean delivery rates, or in perinatal outcomes. so that the use of the Foley catheter was as effective as misoprostol for cervical ripening (14).
In 2011, Cromi, Ghezzi, Uccella, Agosti, Serati, Marchitelli and Bolis conducted a study whose purpose was to determine whether the maximum time for cervical ripening (12-24hours) is influenced by the insertion of a transcervical Foley catheter, in addition to comparing its efficacy versus intravaginal PGE-2. The authors concluded that there was a higher proportion of women who achieved vaginal delivery compared to those who had the balloon for only 12 hours, not to mention that it had a slightly higher efficacy than prostaglandins (15). We also obtained similar results to the previously mentioned investigations, where 65.4% of the total number of patients achieved ripening and labor onset.
In 2011, Fox, Saltzman, Roman, Klauser, Moshier, and Rebarber published a meta-analysis in the British Journal of Obstetrics and Gynecology comparing the use of intravaginal misoprostol and Foley catheters. They concluded that both methods are effective in inducing labor; however, the transcervical Foley catheter was associated with a lower incidence of tachysystole (16).
In the same year, Jozwiak, Oude, Ten Eikelder, van Pampus, Dijksterhuis, de Graaf, van der Post, van der Salm, and Scheepers conducted a randomized controlled trial comparing the effectiveness and safety of the Foley catheter versus the use of intravaginal misoprostol. They concluded that there were no differences in cesarean section rates, and that there was less uterine hyperstimulation, changes in fetal heart rate, and instrumental delivery rates with the use of the Foley catheter, so the use of the catheter may have greater advantages than misoprostol (17).
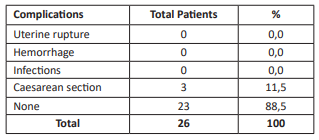
Without a doubt, these are just two studies comparing the use of the balloon with one of the alternative pharmacological methods, both demonstrating a low incidence of complications. In our opinion, there were no fetal complications, since the cause of the Foley catheter use was intrauterine fetal death. In the three patients who underwent cesarean section, the primary cause was method failure. This represented only 11.5%.
Conclusions
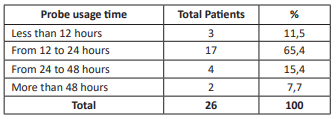
In our study, the success rate for vaginal delivery averaged 88.5%, with 50% of the study sample occurring in the third trimester. As a favorable factor, more than half of the sample had one or more previous vaginal deliveries as an obstetric history. Only 15.4% of the total had a Bishop score of three points as an unfavorable factor. The time from catheter placement to vaginal delivery averaged 24 hours, which is consistent with data reported by many other authors. As an encouraging finding, and also in line with the results of other research, only 11.5% of patients required cesarean delivery due to failure of the method used in the study, with no reports of uterine rupture, hemorrhage, or secondary infections. Given the lower risk of uterine hyperstimulation, the Foley catheter appears to be an effective and safe method for cervical ripening and induction of labor in cesarean sections. Given the small study population, we believe it is important to conduct a study with a larger sample size to demonstrate with greater statistical weight the efficacy and safety of the Foley catheter for cervical ripening and labor induction.