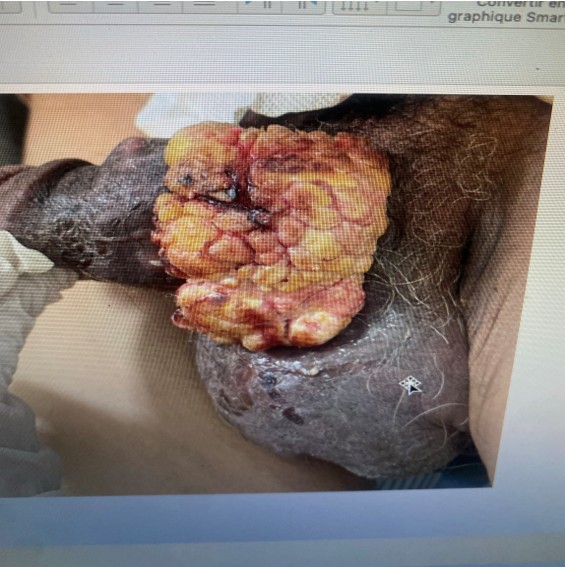
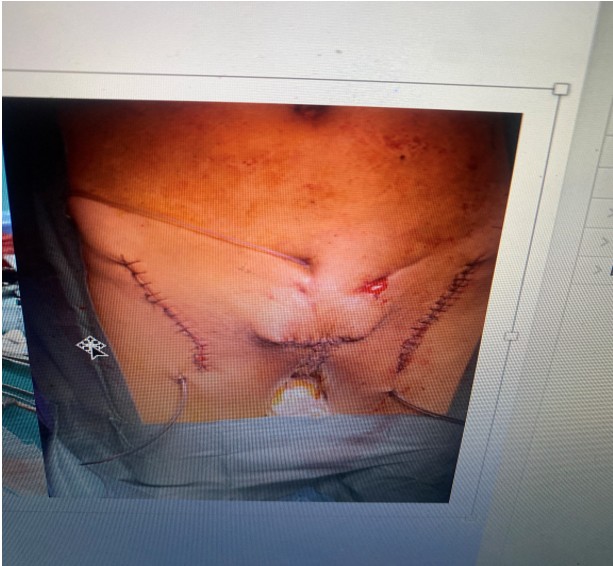
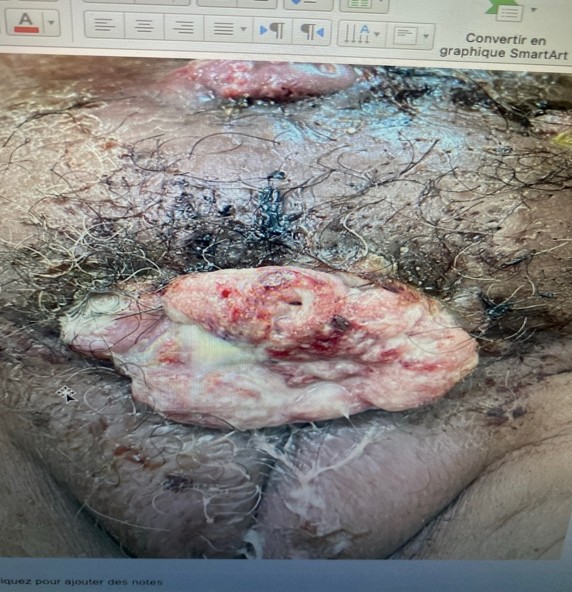
Buschke-Löwenstein tumor, also called giant condyloma acuminatum, is a rare tumor lesion of viral origin, linked to chronic infection by human papillomaviruses (HPV), most often types 6 and 11. It preferentially affects immunocompromised individuals or those with risk factors such as poor hygiene, unprotected sexual intercourse, or a history of sexually transmitted infections [1]. Although histologically benign at its onset, this tumor can exhibit slow but invasive growth, leading to significant local destruction and malignant degeneration in 30 to 50% of cases [2,3]. Treatment is based on wide, sometimes mutilating, surgical excision. Recurrences are frequent, and the prognosis depends on the degree of locoregional spread and the differentiated nature of the carcinoma. We report here a particularly aggressive form, with recurrence after emasculation.
In addition to its anatomical implications, this condition has a significant psychological and social impact, particularly in advanced forms requiring mutilating procedures such as emasculation. The overall prognosis is linked to the stage at diagnosis, the effectiveness of surgical excision, and rigorous postoperative monitoring to prevent frequent recurrences.
istologically, Buschke-Löwenstein tumor is distinguished by its papillomatous architecture, marked acanthosis, and significant hyperkeratosis. It is characterized by the absence of significant cellular atypia at the onset, which can delay diagnostic suspicion. However, its slow but invasive exophytic growth is often accompanied by major tissue destruction, making its surgical treatment complex.
Epidemiologically, BLT primarily affects men between the ages of 40 and 70 and is more common in resource-limited countries due to limited access to sexual health care and HPV vaccination. The prevalence is also higher in immunocompromised patients, particularly those infected with HIV.
Buschke-Löwenstein tumor (BLT), or giant condyloma acuminatum, is a rare and atypical entity. It presents distinct clinical, histological, and evolutionary characteristics from classic condylomata acuminata. This tumor, although histologically benign at its onset, is recognized for its marked local invasiveness, with destructive potential to surrounding soft tissues, and its high risk of malignant transformation.