Novel STAT3 Mutation in a Patient with Hyper-IgE Syndrome Presenting with Recurrent Pulmonary Infections (Job Syndrome)
Chin Soey1*, Chean Sophâl1, Adli Bin Ali2
¹Department of Pediatric Hematology and Immunology, National Pediatric Hospital, Phnom Penh, Cambodia
²UKM Specialist Children’s Hospital, The National University of Malaysia, KualaLumpur, Malaysia
*Corresponding author
Chin Soey, Department of Pediatric Hematology and Immunology, National Pediatric Hospital, Phnom Penh, Cambodia
DOI: 10.55920/JCRMHS.2025.10.001447
Figure 1: Scars following the recurrent cutaneous infection
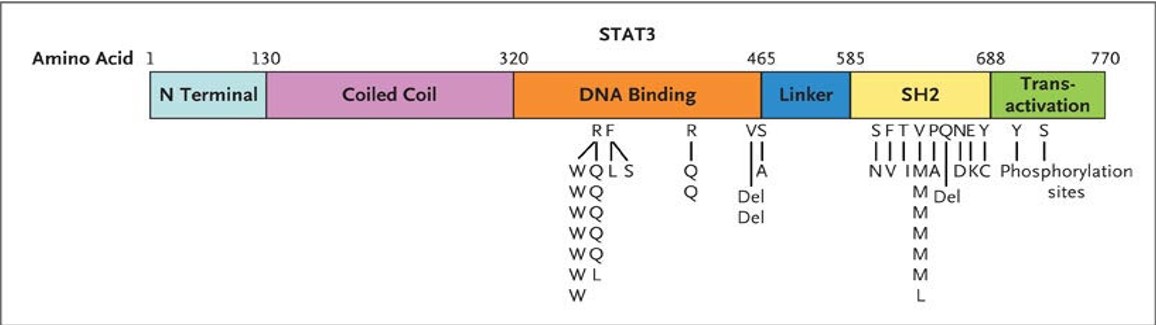
Figure 2: Genomic DNA analysis, STAT3 Mutations
Figure 3: Chest radiograph on admission (A: posteroanterior and B: lateral view) showing multiple thin‐walled cyst (pneumatoceles) with air‐fluid level (*).
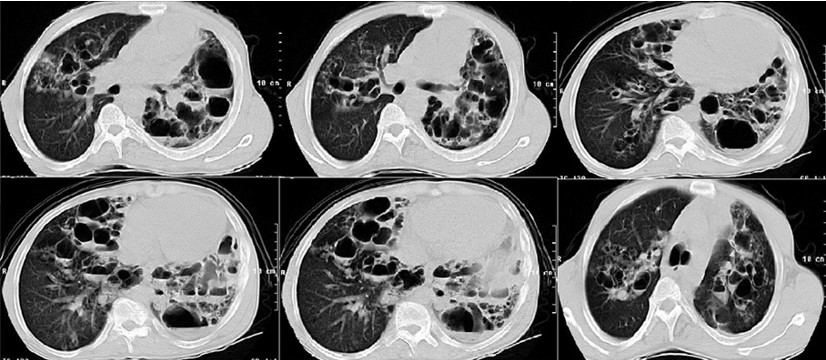
Figure 4: Chest CT scan on admission showed multiple and large pneumatoceles, some with air‐fluid level consistent with superinfection mainly at middle and lower lung fields, mild consolidation, bronchiectasis, and left pleural thickening.
Key Laboratory Findings: Serum IgE: >5000 IU/mL (Elevated, highly suggestive of an atopic phenotype), NIH AD-HIES score: 45 (Highly suggestive of Job Syndrome), LPT (Lymphocyte Proliferation Test): Reduced compared to controls (Impaired T-cell proliferation), SAR (Specific Antibody Response): Normal response to tetanus toxoid and pneumococcal vaccines, Genetic Analysis: Pathogenic heterozygous STAT3 mutation (confirming the diagnosis of Job Syndrome)
Infection History: Neonatal period: Congenital pneumonia requiring CPAP, Childhood: Multiple episodes of pneumonia, RSV infection, and mycoplasma pneumonia, Recurrent abscesses (including MSSA-positive shoulder and cervical lymphadenitis), Fungal infections: Onychomycosis, oral candidiasis, Aspergillus niger detection, Bronchiectasis: Diagnosed at age 5 via HRCT thorax (right middle lobe bronchiectasis).
Immunological & Functional Studies
STAT3 Expression: Normal despite a pathogenic mutation, a common feature of Job Syndrome, Neutrophil Oxidative Burst Assay (DHR): Normal (indicating that neutrophil function is intact), LPT: Reduced response to mitogens (suggesting impaired T-cell proliferation), Isohemagglutinin Titers: Elevated, supporting immune dysregulation.
Management and Treatment
Prophylactic antibiotics: Trimethoprim-sulfamethoxazole (Bactrim) 130 mg every other day (EOD)
Antifungal prophylaxis: Itraconazole 100 mg OD
Bronchodilator therapy: Salbutamol MDI as needed (PRN)
Corticosteroid inhaler: Fluticasone (discontinued in November 2021)
Immunology follow-ups: Every two months, Pulmonary management: Bronchoscopy lavage used for pulmonary infections.
Discussion and Diagnosis: This patient presents with clinical and laboratory features highly suggestive of Hyper-IgE Syndrome (Job Syndrome), which is characterized by: Severe eczema, Recurrent skin abscesses, Elevated IgE levels, Recurrent respiratory infections, STAT3 mutation (autosomal dominant) confirming the diagnosis.
The elevated serum IgE (>5000 IU/mL), reduced T-cell proliferation (LPT), and the NIH AD-HIES score (45) are all critical in leading to the diagnosis. The patient has a history of recurrent bacterial, viral, and fungal infections, which are typical in Job Syndrome due to impaired immunity, specifically related to T-cell dysfunction.
Management and Prognosis: While there is no definitive cure for Job Syndrome, management focuses on Prophylactic antibiotics and antifungal treatment to reduce infection risk. Pulmonary care to manage recurrent respiratory infections and bronchiectasis. Regular immunology follow-ups to monitor immune function and prevent infections. The prognosis varies depending on the severity of the condition and the presence of complications. Early interventions and preventive treatments significantly improve outcomes and quality of life.
Differential Diagnosis: Given the complexity of the patient's clinical presentation, the differential diagnosis for her symptoms may include Severe Combined Immunodeficiency (SCID) SCID can present with recurrent infections and eczema, but the reduced lymphocyte proliferation test (LPT) and the genetic confirmation of STAT3 mutation steer the diagnosis toward Job Syndrome rather than SCID. Wiskott-Aldrich Syndrome (WAS) Similar presentation with eczema, recurrent infections, and immune dysregulation, but typically, WAS presents with thrombocytopenia, which was not noted in this patient. Chronic Granulomatous Disease (CGD) Recurrent infections due to neutrophil dysfunction, but the normal DHR assay helps exclude CGD in this case. Atopic Dermatitis While the patient’s eczema is prominent, the associated recurrent infections, elevated IgE levels, and genetic findings make Job Syndrome more likely than simple atopic dermatitis.
Genetics of Job Syndrome:
STAT3 Mutation: This genetic mutation is key to the diagnosis of Autosomal Dominant Hyper-IgE Syndrome (AD-HIES). STAT3 plays a crucial role in immune response regulation, and a mutation here leads to the characteristic immune dysregulation seen in Job Syndrome, including defects in T-helper cell function and increased susceptibility to infections. Inheritance: The patient has a heterozygous mutation in STAT3, which means the condition is inherited in an autosomal dominant manner. This suggests that one affected parent could pass on the mutation, but genetic testing of the parents was negative.
Treatment Rationale: Prophylactic Antibiotics (Bactrim): Regular use helps prevent bacterial infections, particularly pneumonia, which is common in patients with Job Syndrome due to impaired immune function.
Antifungal Prophylaxis (Itraconazole): Fungal infections, such as candidiasis and Aspergillus, are common in Job Syndrome. Itraconazole is used to prevent these infections. Bronchodilator
Therapy: For the management of recurrent respiratory infections and to ease any bronchospasm that may occur, particularly in the context of bronchiectasis.
Inhaled Corticosteroids (Fluticasone): Discontinued in November 2021, possibly due to a concern over the side effects or ineffectiveness in the context of her underlying immune dysregulation.
Immunology Follow-ups: Regular monitoring is important to track the development of infections and adjust treatment protocols, ensuring optimal management of immune deficiencies.
Bronchoscopy Lavage: Used as part of the management of pulmonary infections. This less invasive approach may prevent the need for more aggressive treatments such as surgery.
Complications and Prognosis Infections: Recurrent infections (respiratory, skin abscesses, fungal) are a major concern. Early prophylactic treatment is key to improving outcomes.
Bronchiectasis: Already present in this patient, this condition could progressively worse if infections are not adequately managed.
Growth and Development: Children with Job Syndrome can sometimes experience growth delays or developmental issues due to recurrent infections and immune dysregulation. This case emphasizes the importance of recognizing the signs of Hyper-IgE Syndrome (Job Syndrome) early, especially when recurrent infections, eczema, and immune dysregulation are present. The genetic confirmation of a STAT3 mutation helps solidify the diagnosis, guiding management decisions such as prophylactic antibiotics and antifungal treatments, as well as regular immunology follow-ups. Early intervention and ongoing care can improve quality of life and prevent severe complications like recurrent infections and progressive bronchiectasis.