Sickle cell nephropathy, a complication not to be ignored, through a Moroccan case
Asmaa Biaz1,3 , Imane Ouiazza1,3 , Leila Laamara1,3 , Abdelaali Bahadi2,3 ,Sanae Bouhsain1,3,Driss ELKabbaj2,3,Abdellah Dami1,3,Samira Elmachtaniidrissi1,3
1Biochemistry-Toxicology Department, Mohammed V Military Training Hospital, Rabat,Morocco
2Nephrology Department, Mohammed V Military Training Hospital, Rabat,Morocco
3Faculty of Medicine and Pharmacy, Mohammed V University in Rabat, Morocco
*Corresponding author
*Asmaa Biaz, Biochemistry-Toxicology Department, Mohammed V Military Training Hospital, Rabat,
Morocco
E-mail: biazasmaa@yahoo.fr
DOI: 10.55920/JCRMHS.2022.01.001025
Figure 1: Electrophoretic profile of the patient uninterpretable due to recent transfusion
Figure 2: Electrophoretic profile of the mother showing hemoglobinosis O-Arab in the heterozygous state
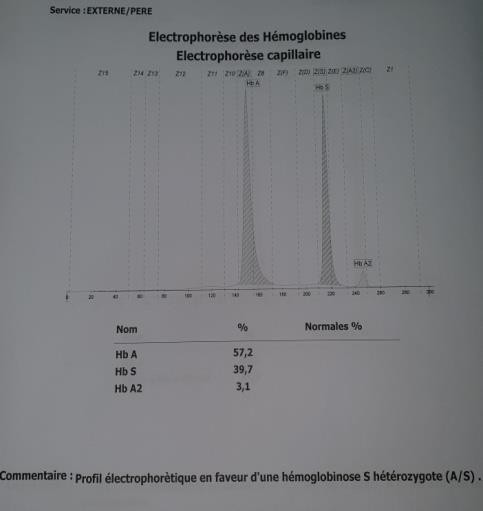
Figure 3: Electrophoretic profile of the father showing hemoglobinosis S in the heterozygous state
Referring to the phenotypic study of Hb performed in the parents, it is concluded that the patient has a composite heterozygosity S/O-Arab explaining the severity of the renal manifestations.
The evolution was marked by the absence of improvement of her renal function and the aggravation of the uremic syndrome motivating her setting in peritoneal dialysis. The patient was treated with erythropoietin ARANESP 30µg/ per 2 weeks with a blood transfusion of 2 packed red blood cells on average every two months.
The patient died at the age of 26 years before benefiting from either a hemoglobin genotyping study or a renal transplant.
- Hariri E , Mansour A , El Alam A, Daaboul Y , Korjian S , Bahous SA. Néphropathie drépanocytaire : une mise à jour sur la physiopathologie, le diagnostic et le traitement. Int Urol Néphrol. Juin 2018; 50(6):1075-1083. PMID: 29383580.
- Piel FB, Patil AP, Howes RE, Nyangiri OA, Gething PW, Dewi M, et al. Global epidemiology of sickle haemoglobin in neonates: acon temporary geostatistical model-based map and population estimates. Lancet 2013;381: 142-51. PMID: 23103089.
- Hafsia R, Meddabb B, Ayari M, Hafsia A, Boussen M. Association hémoglobine O Arab/hémoglobine S : à propos de 3 cas. Tunis Med 1991; 69 (3):171-5. PMID: 1841472.
- Nath KA, Hebbel RP. Sickle cell disease: renal manifestations and mechanisms. Nat Rev Nephrol 2015. PMID : 25668001.
- McClellan AC, Luthi JC, Lynch JR, Soucie JM, Kulkarni R, Guasch A, et al. High one year mortality in adults with sickle cell disease and end-stage renal disease. Br J Haematol 2012;159:360–7. PMID : 22967259.
- Becker AM (2011) Sickle cell nephropathy: challenging the conventional wisdom. Pediatric Nephrol 26:2099–2109. PMID: 21203778
- Nath KA, Katusic ZS (2012) Vasculature and kidney complications in sickle cell disease. J Am Soc Nephrol 23:781–784 PMID: 22440903.
- Gonzalez-Michaca L, Farrugia G, Croatt AJ, Alam J, Nath KA(2004) Heme: a determinant of life and death in renal tubular epithelial cells. Am J Physiol Renal Physiol 286:F370–F 377. PMID: 14707007.
- Juncos JP, Grande JP, Croatt AJ, Hebbel RP, Vercellotti GM, Katusic ZS et al (2010) Early and prominent alterations in hemodynamics, signaling, and gene expression following renal ischemia in sickle cell disease. Am J Physiol Renal Physiol 298:F892–F 899. PMID : 20107113.
- Bouanani N., EL Bakkouri J., Faez S., Benchemsi N. L’atteinte rénale chez les patients drépanocytaires. Les technologies de laboratoire - 2013, Volume 8, N°31. https://revues.imist.ma/index.php/technolab/article/download/726/600